Patients diagnosed with a malignancy frequently assume that their medical journey will involve a single, predetermined medical intervention. However, modern oncology utilizes highly complex, sequenced protocols.
Whether a patient requires advanced Chemotherapy treatment in Bangalore or highly targeted Immunotherapy treatment in Bangalore, the clinical strategy is never generic.
As a leading Cancer Treatment Hospital in Bangalore and widely recognized as the Best Cancer Hospital in Bangalore, Dasappa Cancer Hospital relies on an extensive multidisciplinary evaluation before initiating any therapy. Navigating this critical phase often leads patients to ask exactly how a medical team formulates a customized treatment plan for a cancer patient.
Historically, physicians relied heavily on broad surgical resections or generalized systemic treatments based solely on the anatomical origin of the tumor.
Today, developing an optimal clinical strategy requires analyzing a massive volume of highly specific pathological and physiological data. Understanding how this complex medical decision is made requires examining three specific dimensions of oncological planning:
- The Diagnostic Foundation: Defining how precise tumor staging and pathological grading strictly dictate the aggressiveness of the required medical intervention.
- The Multidisciplinary Review: Explaining how diverse oncology specialists collaborate to prevent single modality biases and ensure comprehensive, integrated care.
- The Therapeutic Selection: Outlining how physicians evaluate different medical modalities to construct a highly sequenced, individualized protocol.
With the meticulous methodology behind these clinical decisions, patients can confidently participate in their own medical care and understand the precise rationale driving their specific therapeutic trajectory.
The Diagnostic Foundation of Pathology and Staging
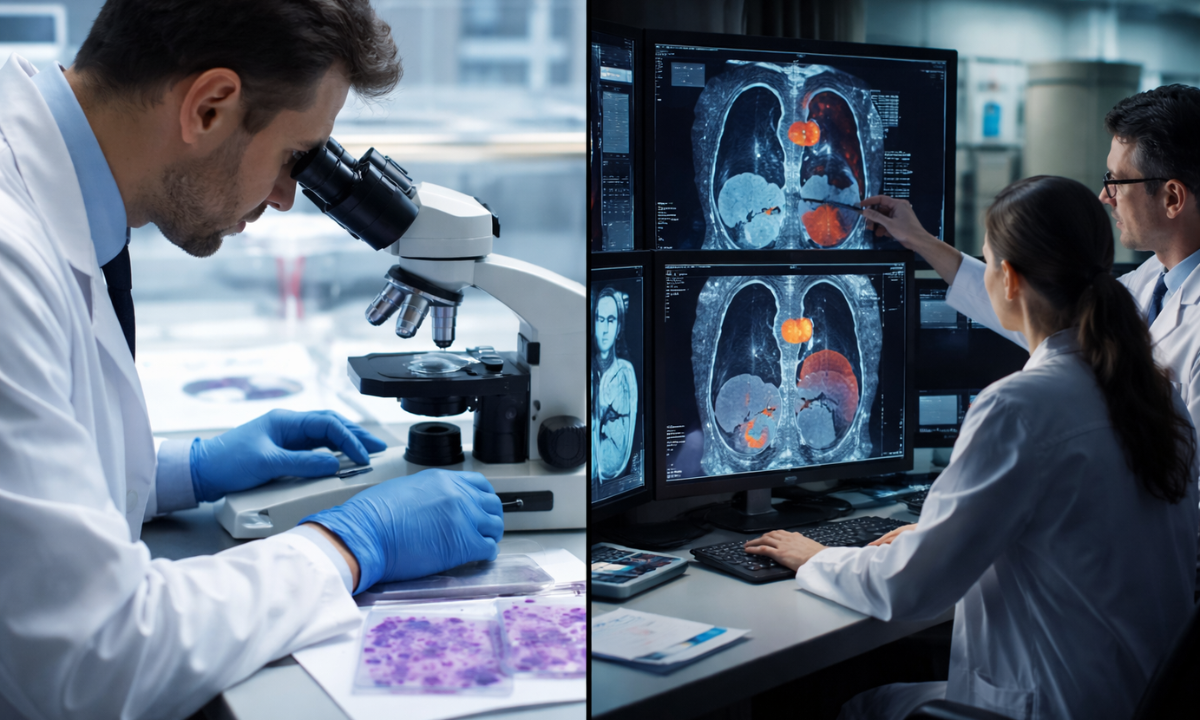
Before any medical intervention begins, the multidisciplinary tumor board strictly requires a definitive pathological diagnosis and an accurate anatomical staging.
This diagnostic data serves as the absolute foundation for the entire clinical strategy. A medical protocol is never formulated based on a preliminary clinical suspicion; it requires microscopic confirmation and precise anatomical mapping.
The diagnostic foundation consists of two primary clinical pillars:
1. Pathological Grading: Following a surgical biopsy, a clinical pathologist analyzes the extracted tissue under a high-resolution microscope. The pathologist determines the exact cellular classification of the tumor and its specific histological grade.
The grade indicates how closely the malignant cells resemble normal healthy tissue and strictly predicts the biological aggressiveness of the disease. A high-grade tumor replicates rapidly and demands a significantly more aggressive immediate medical response.
2. Anatomical Staging (The TNM System): Once the malignancy is confirmed, the oncology team utilizes advanced radiological imaging, such as PET scans or high-resolution CT scans, to determine the exact physical extent of the disease. This is universally quantified using the TNM staging system:
- T (Tumor): Evaluates the primary anatomical size and the precise physical depth of the primary tumor penetration into the surrounding localized tissue.
- N (Node): Determines whether the malignant cells have physically migrated into the adjacent regional lymphatic system.
- M (Metastasis): Assesses whether the primary malignancy has spread through the bloodstream to establish secondary tumors in distant anatomical organs.
Combining the microscopic pathological grade with the macroscopic TNM stage, the medical team definitively categorizes the severity of the malignancy.
This highly specific categorization is strictly required to determine whether the patient is a candidate for immediate surgical resection or if they require preliminary systemic therapies to shrink the tumor before any surgical intervention.
The Multidisciplinary Tumor Board of Collaborative Medicine
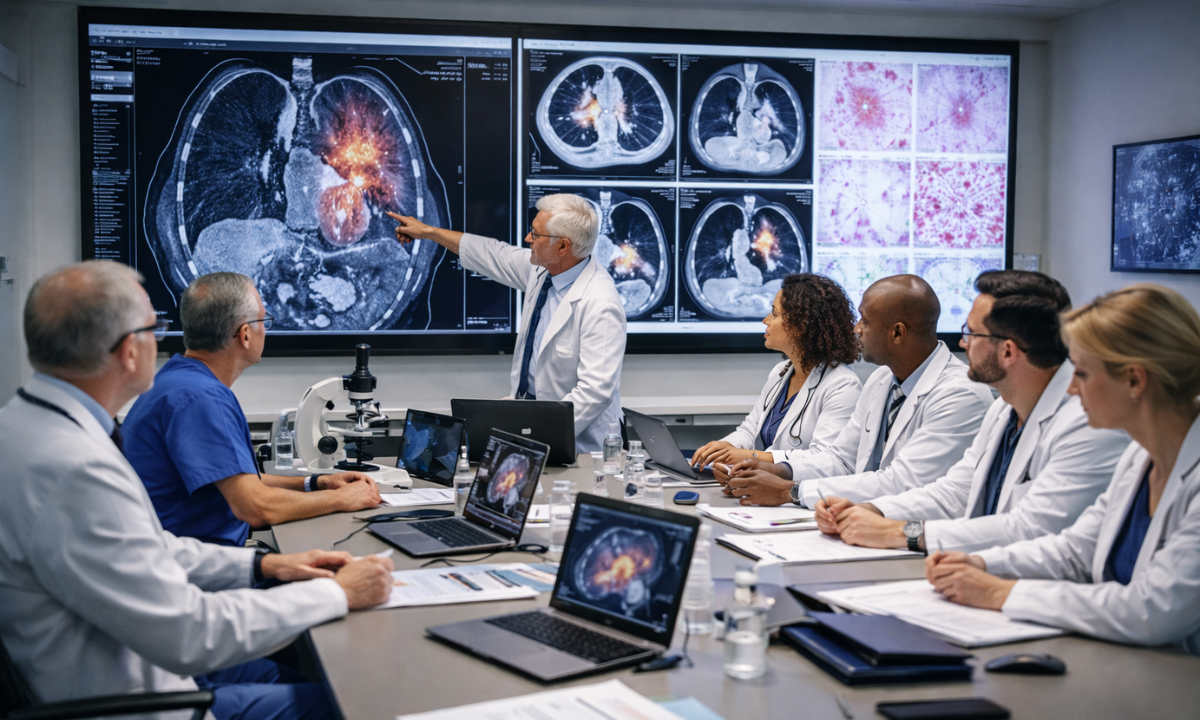
Following the initial diagnostic and staging phase, the clinical data is not reviewed by a single physician in isolation.
Modern oncological care in medicine strictly mandates a collaborative review process conducted by a highly specialized group of medical experts known as the Multidisciplinary Tumor Board. This collaborative approach is strictly engineered to completely eliminate single modality bias and ensure that every available therapeutic option is objectively evaluated.
The tumor board consists of several distinct clinical specialists, each analyzing the patient data from their specific medical discipline:
- Surgical Oncologists: Evaluate the precise anatomical location and physical boundaries of the tumor to determine if complete structural resection is a viable and clinically safe initial option.
- Medical Oncologists: Analyze the specific molecular and cellular pathology to determine the strict necessity of systemic treatments, including advanced intravenous chemotherapy or targeted immunotherapy protocols.
- Radiation Oncologists: Assess the localized physical extent of the malignancy to evaluate the potential efficacy of highly targeted radiation therapy to actively shrink the tumor or eliminate residual microscopic disease.
- Clinical Pathologists and Radiologists: Provide the absolute foundational diagnostic interpretation, ensuring the surgical and medical teams possess the most accurate cellular and anatomical data before making therapeutic decisions.
Reviewing the clinical data simultaneously, these specialists collaboratively sequence the medical interventions. They determine the precise order of treatments, such as administering systemic chemotherapy before surgery to physically shrink the tumor mass, clinically referred to as neoadjuvant therapy, or prescribing targeted radiation following surgery to definitively eliminate any remaining microscopic malignant cells, known as adjuvant therapy.
This highly integrated medical collaboration guarantees the formulation of the most comprehensive and clinically effective strategy for the patient.
Which Treatment Is Best for Cancer?
When patients first consult with a medical oncologist, they frequently ask exactly which treatment is best for cancer. In modern oncology, there is absolutely no universal standard of care that applies to all malignancies.
The optimal therapeutic intervention is never a singular choice but rather a highly customized selection of medical modalities based entirely on the precise pathological data and anatomical staging.
The multidisciplinary tumor board selects from several primary therapeutic pillars. Each medical modality possesses a distinct biological objective and a highly specific mechanism of action.
Primary Clinical Modalities in Medical Oncology
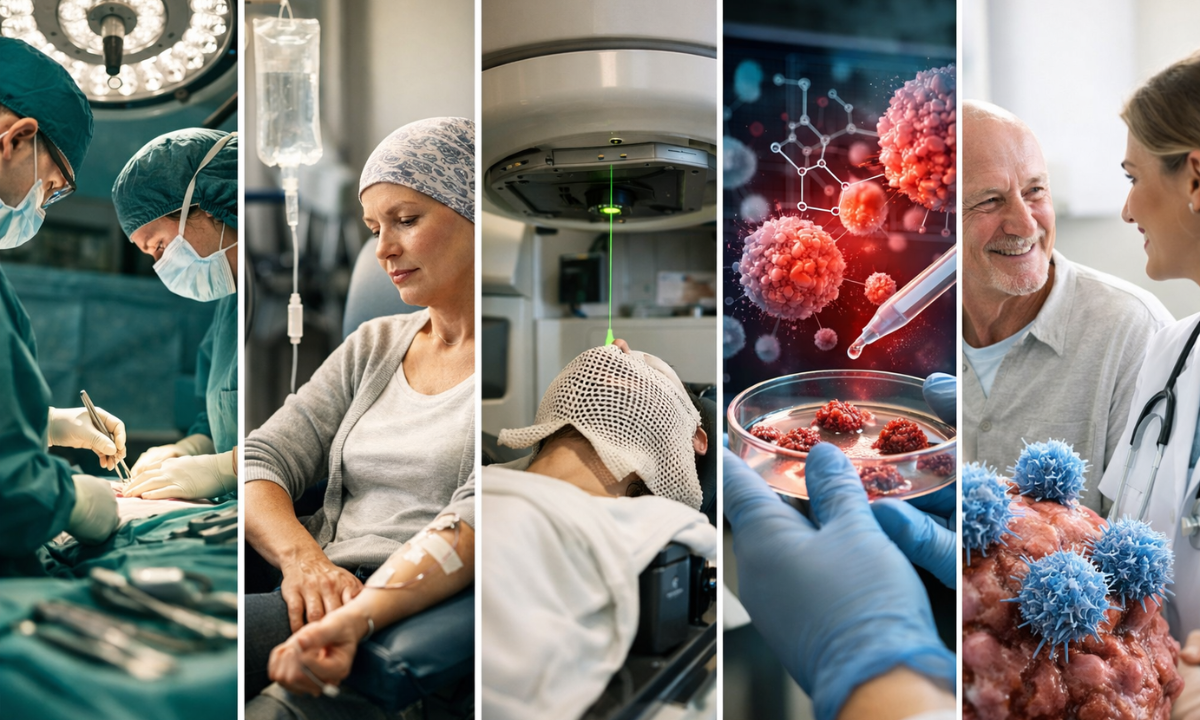
| Therapeutic Modality | Primary Clinical Objective | Mechanism of Action |
|---|---|---|
| Surgical Resection | To physically eradicate the primary malignant tumor from the localized anatomical site. | The surgical oncologist physically extracts the solid tumor mass and the immediately surrounding healthy tissue margins to prevent localized disease recurrence. |
| Systemic Chemotherapy | To systematically destroy rapidly dividing malignant cells distributed throughout the entire body. | Intravenous cytotoxic agents circulate directly through the bloodstream to neutralize widespread microscopic metastasis and physically shrink primary tumors before surgical intervention. |
| Radiation Therapy | To precisely target and destroy localized malignant tissue utilizing high-energy photon beams. | Advanced linear accelerators deliver highly concentrated ionizing radiation directly to the tumor bed, fundamentally destroying the internal DNA of the malignant cells and strictly preventing further cellular replication. |
| Targeted Therapy | To precisely disrupt the specific molecular pathways driving the cellular growth of the tumor. | Specialized oral or intravenous pharmaceutical agents physically bind to mutated proteins or receptors on the cancer cell, effectively halting the oncogenic signaling pathway without severely damaging adjacent normal tissue. |
| Immunotherapy | To artificially stimulate the patient’s immune system to actively recognize and destroy malignant cells. | Advanced immune checkpoint inhibitors block the specific deceptive surface proteins that tumors utilize to hide from the immune system, thereby authorizing a robust natural immune response against the disease. |
These advanced medical interventions are rarely deployed in strict isolation. The oncology board meticulously sequences these modalities.
The team may administer systemic chemotherapy to shrink a large tumor before a complex surgical procedure, or they may prescribe localized radiation therapy following a surgical extraction to permanently eradicate any remaining microscopic cellular disease.
This highly integrated sequencing guarantees the maximum possible statistical probability of long-term clinical survival.
Cervical Cancer and Lung Cancer
While the foundational therapeutic modalities remain consistent across the discipline of medical oncology, their precise clinical application varies drastically depending on the exact anatomical origin of the tumor.
To illustrate this profound clinical divergence, the multidisciplinary tumor board executes entirely different sequencing strategies for localized pelvic malignancies compared to complex thoracic diseases.
Pelvic Oncology: Cervical cancer
The clinical management of cervical malignancies frequently prioritizes highly aggressive localized interventions.
As these specific tumors are anatomically confined within the pelvic cavity during their early and intermediate stages, the primary medical objective is complete localized destruction.
1. Concurrent Chemoradiation: The definitive standard protocol for locally advanced disease involves administering systemic intravenous chemotherapy simultaneously with high-energy external beam radiation.
In this specific scenario, the chemotherapy acts strictly as a radiosensitizer. It chemically alters the malignant pelvic cells to make them significantly more vulnerable to the targeted radiation beams.
2. Brachytherapy Integration: Following external radiation, radiation oncologists frequently utilize advanced internal brachytherapy.
This precise procedure involves temporarily placing a radioactive isotope directly inside the cervical anatomy. This delivers a massive localized dose of radiation to the residual tumor tissue while strictly sparing the adjacent healthy bladder and bowel structures.
Thoracic Oncology: Lung cancer
Conversely, the clinical strategy for pulmonary malignancies, including lung cancer, relies heavily on systemic and molecular interventions. As the thoracic cavity is highly vascular and pulmonary tumors frequently exhibit early microvascular spread, localized structural therapy alone is often clinically insufficient.
1. Genomic Sequencing Mandate: Before formulating any medical protocol, pathologists must perform a comprehensive molecular analysis of the extracted tumor tissue.
This strictly determines if the malignancy is driven by specific genetic mutations.
2. Systemic and Targeted Dominance: Based strictly on the genomic data, medical oncologists deploy highly specific oral targeted therapies or advanced intravenous immune checkpoint inhibitors.
If the tumor remains strictly localized, thoracic surgeons may perform a precise anatomical lobectomy to extract the diseased pulmonary lobe. This surgical extraction is frequently followed by systemic adjuvant therapy to definitively neutralize any undetected circulating malignant cells.
To further clarify this strategic divergence, the following matrix outlines the contrasting clinical priorities between these two distinct oncology disciplines.
Clinical Comparison of Site-Specific Treatment Sequencing
| Clinical Parameter | Cervical Cancer (Pelvic Malignancy) | Lung Cancer (Thoracic Malignancy) |
|---|---|---|
| Primary Diagnostic Focus | Anatomical staging and precise physical tumor volume measurement. | Comprehensive molecular profiling and specific genetic mutation identification. |
| Dominant Local Intervention | Radical surgical excision or aggressive concurrent chemoradiation protocols. | Anatomical pulmonary lobectomy combined with complete mediastinal lymph node dissection. |
| Advanced Therapeutic Focus | High dose rate internal brachytherapy is applied directly to the anatomical tumor bed. | Oral tyrosine kinase inhibitors or advanced intravenous immunotherapy agents. |
| Primary Clinical Challenge | Eradicating the dense tumor mass while strictly preserving adjacent urological and gastrointestinal organ function. | Controlling rapid systemic microvascular metastasis and overcoming acquired molecular pharmaceutical resistance. |
Utilizing distinct, site-specific clinical protocols, the oncology team ensures that the therapeutic intervention exactly matches the biological behavior and the anatomical location of the specific malignancy.
Why Choose Dasappa Cancer Hospital? Advanced Oncological Care at Dasappa Cancer Hospital
We at Dasappa Cancer Hospital recognize that clinical excellence strictly requires absolute diagnostic precision and unwavering medical collaboration. Formulating an optimal treatment plan is a highly complex process that demands specialized infrastructure and diverse oncological expertise.
By choosing our facility, patients secure direct access to several critical medical advantages:
- Integrated Multidisciplinary Board: Our specialized team of surgical medical, and radiation oncologists reviews every single diagnostic report collaboratively. This ensures that no single medical discipline dominates the treatment strategy and guarantees a truly comprehensive approach.
- Advanced Diagnostic Infrastructure: We utilize state-of-the-art genomic sequencing and high-resolution radiological imaging directly on site. This allows our physicians to accurately stage the malignancy and formulate a highly targeted response without dangerous delays.
- Comprehensive Therapeutic Execution: From advanced minimally invasive surgical resections to highly targeted systemic immunotherapy protocols, our hospital possesses the complete technological capability required to execute the most complex medical strategies.
Choosing Dasappa Cancer Hospital means securing access to a highly sophisticated medical facility where evidence-based protocols and multidisciplinary collaboration strictly dictate your clinical care.
Conclusion
Receiving a cancer diagnosis initiates a highly complex medical journey. However, understanding how doctors formulate a customized treatment plan empowers patients to actively participate in their own clinical care.
The selection of surgical systemic, or radiation therapies is never random. It is a meticulously calculated medical decision based entirely on precise pathological data and anatomical staging.
If you require a comprehensive oncological evaluation or a definitive second medical opinion regarding a complex malignancy, contact Dasappa Cancer Hospital today.
Schedule a consultation with our multidisciplinary tumor board to secure a precisely sequenced treatment protocol designed specifically to optimize your long term clinical outcome.