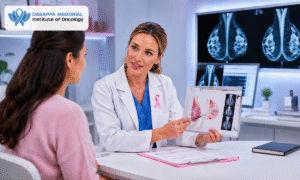
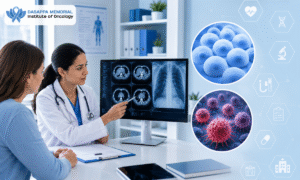
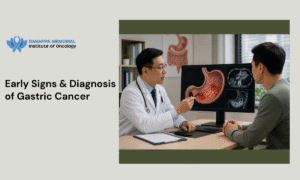
Receiving a complex oncology diagnosis requires immediate and comprehensive medical intervention. Patients seeking an advanced Cancer Hospital in Bangalore often focus entirely on curative therapies, such as surgical resection or aggressive chemotherapy.
However, achieving optimal clinical outcomes requires addressing the severe physiological and emotional toll of the disease itself. As the Best Cancer Hospital in Bangalore, Dasappa Cancer Hospital prioritizes comprehensive symptom management alongside curative protocols. Integrating specialized palliative care treatment for cancer patients from the point of initial diagnosis is clinically proven to significantly improve a patient’s overall quality of life.
Accessing expert palliative care bangalore ensures that every physical burden is actively managed.
A widespread clinical misconception persists among patients and their families that accepting palliative support signifies a cessation of active medical treatment. In modern oncology, this is factually incorrect.
Supportive care is a highly active, concurrent medical discipline designed to maximize patient comfort and functional independence at any stage of a life threatening illness. It provides an essential layer of specialized medical support that operates in tandem with primary cancer treatments.
To provide clear, evidence based guidance on this vital aspect of oncology, this clinical guide will systematically detail the specific medical protocols involved in supportive care, addressing the following critical components:
- Defining the Clinical Scope: We will clarify the exact medical objectives of supportive interventions and clearly differentiate them from end of life hospice care.
- Mapping the Stages of Care: We will outline the structured progression of symptom management from the initial cancer diagnosis through advanced disease progression.
- The Multidisciplinary Approach: We will detail the specific roles of the specialized medical professionals who deliver these critical daily therapeutic interventions.
Understanding the precise clinical definition and the profound benefits of early integration, patients can proactively utilize these specialized support systems to maintain their physical and emotional resilience throughout their oncology treatment.
The Clinical Definition of Palliation in Cancer
To fully utilize supportive oncology services, patients must first understand their exact medical scope. According to the foundational clinical guidelines established by the World Health Organization, palliative care is defined as a specialized medical approach that explicitly improves the quality of life of patients and their families facing the profound challenges associated with life threatening illnesses.
The primary biological and psychological objective is the prevention and relief of suffering through early identification, impeccable clinical assessment, and the targeted treatment of pain and other systemic complications.
The most critical clinical distinction to establish is the fundamental difference between palliative oncology and hospice care. While all hospice care utilizes palliative principles, not all palliative care is hospice. Hospice care is strictly restricted to the terminal phase of an illness when all curative interventions have ceased entirely.
Conversely, palliation in cancer is actively administered concurrently with disease modifying therapies. A patient actively receiving aggressive surgical resection, heavy chemotherapy, or targeted radiation is simultaneously eligible for full palliative support.
The clinical framework of supportive oncology is systematically built upon three primary pillars of patient management:
Physical Symptom Management
The medical team aggressively treats both the direct physiological consequences of the growing malignancy and the toxic, systemic side effects of the cancer treatments.
This includes the precise pharmacological management of severe pain, chronic chemotherapy induced nausea, cancer cachexia (extreme involuntary weight loss), respiratory distress, and profound neurological fatigue.
Psychological and Cognitive Support
Clinical psychologists and specialized oncology counselors directly address the severe cognitive burdens associated with a major cancer diagnosis.
Therapeutic interventions are highly structured to manage clinical depression, severe anxiety disorders, and the specific emotional distress and anticipatory grief experienced by the patient’s primary caregivers and immediate family members.
Spiritual and Existential Care
Dedicated spiritual care providers assist patients in navigating the profound existential crises that frequently accompany life threatening diagnoses.
This support ensures that all advanced medical directives and ongoing treatment decisions strictly align with the patient’s personal, cultural, and spiritual value systems.
Formally defining these three pillars, the medical team ensures that no aspect of the patient’s suffering is overlooked during their curative treatment timeline.
Navigating the Palliative Care 5 Stages
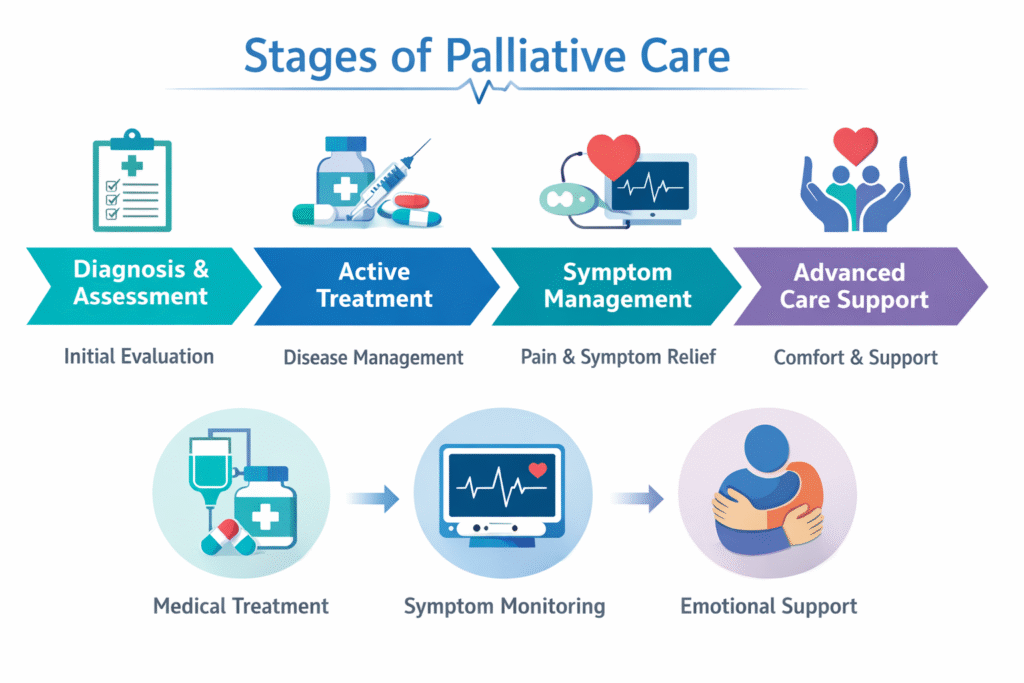
To effectively manage the severe physical and emotional complexities of a cancer diagnosis, clinical oncology utilizes a highly structured, phased approach to supportive care.
Understanding the palliative care 5 stages allows patients and their primary caregivers to accurately anticipate the level of medical intervention required as the disease and its subsequent treatments progress.
This formalized framework ensures that the multidisciplinary medical team dynamically adjusts their pharmacological and psychological support to match the patient’s exact physiological state at any given time.
The progression of supportive oncology is officially categorized into the following distinct clinical phases:
The Clinical Progression of Supportive Oncology
| Clinical Stage | Primary Medical Focus | Standard Therapeutic Interventions |
| Stage 1: Stable Phase | Initial Assessment and Care Planning. | Establishing a baseline for symptom management, formally defining the patient’s long term care goals, and initiating introductory psychological support concurrently with the start of active curative treatments. |
| Stage 2: Unstable Phase | Acute Symptom Exacerbation Management. | Rapidly adjusting pharmacological protocols to address sudden spikes in severe pain, intractable nausea, or sudden respiratory distress caused by disease progression or extreme treatment toxicity. |
| Stage 3: Deteriorating Phase | Intensive Physiological and Functional Support. | Managing compounding physical decline, preventing severe clinical complications such as secondary infections, and facilitating detailed, medically guided discussions regarding advanced clinical directives. |
| Stage 4: Terminal Phase | Comprehensive End of Life Comfort Care. | Transitioning strictly to hospice protocols, prioritizing absolute physical comfort, actively managing terminal delirium, and officially ceasing all disease modifying therapies. |
| Stage 5: Bereavement Phase | Ongoing Family and Caregiver Support. | Providing structured, long term psychological counseling and targeted grief support services for the immediate family members following the patient’s passing. |
It is critical to note that this specific clinical progression is rarely strictly linear. Patients frequently transition back and forth between the stable and unstable phases depending entirely on their physiological response to ongoing chemotherapy, surgical interventions, or targeted radiation.
Formally categorizing these highly specific stages, the medical team guarantees that the intensity and scope of the palliative support precisely match the patient’s immediate and evolving clinical requirements.
Palliative Care for Stage 3 Cancer
When oncologists diagnose a locally advanced malignancy, clinical protocols strictly mandate aggressive, multimodality therapeutic interventions.
Patients presenting with stage 3 cancer typically require a rigorous combination of systemic chemotherapy, targeted radiation, and extensive surgical resection. Because these curative treatments induce severe physiological toxicity, initiating early palliative care for stage 3 cancer is recognized as a fundamental standard of modern oncology.
Historically, physicians delayed supportive interventions until curative options were exhausted. However, contemporary clinical data confirms that integrating specialized symptom management directly at the time of an advanced diagnosis significantly improves overall survival rates.
This improvement occurs because effective symptom management allows patients to physically tolerate and successfully complete their prescribed chemotherapy and radiation cycles without requiring dangerous, unplanned treatment interruptions.
The integration of supportive oncology during this highly intensive treatment phase specifically addresses three major physiological challenges:
- Cumulative Treatment Toxicity: The simultaneous administration of multiple oncological therapies exponentially increases the severity of systemic side effects, particularly intractable gastrointestinal distress and profound immunosuppression.
- Tumor Mass Effect: Locally advanced tumors physically compress adjacent internal organs, major blood vessels, and dense nerve plexuses. This mechanical compression causes acute, highly localized pain syndromes that require specialized pharmacological management beyond standard over the counter analgesics.
- Severe Nutritional Depletion: Aggressive radiation and systemic chemotherapy frequently induce severe oral mucositis and chronic nausea. These conditions rapidly lead to cancer cachexia, defined as a dangerous, involuntary loss of total body mass and skeletal muscle.
To counteract these specific physiological threats, the multidisciplinary medical team implements targeted therapeutic protocols.
Targeted Palliative Interventions for Advanced Malignancies
| Primary Stage 3 Complication | Targeted Palliative Intervention | Primary Clinical Objective |
| Intractable Chemotherapy Induced Nausea | Implementation of advanced antiemetic pharmacological protocols combined with proactive intravenous hydration therapy. | To prevent severe systemic dehydration and ensure the patient remains physiologically stable for their next scheduled chemotherapy cycle. |
| Acute Malignant Pain Syndromes | Precise clinical titration of opioid analgesics, utilization of transdermal pain patches, and administration of targeted regional nerve block procedures. | To completely neutralize acute pain, restore physical mobility, and ensure the patient can achieve adequate restorative sleep. |
| Severe Cancer Cachexia | Introduction of specialized enteral or parenteral nutritional support pathways combined with pharmacological appetite stimulants. | To aggressively preserve lean muscle mass and optimize the patient’s biological resilience during highly toxic treatment phases. |
Proactively neutralizing these severe physical burdens, the palliative care team directly supports the primary oncology strategy.
This concurrent medical approach guarantees that the patient maintains the maximum biological strength required to endure their curative treatments and actively fight the advancing malignancy.
The Multidisciplinary Team and the Role of Palliative Care Nurse

Delivering highly effective supportive oncology requires far more than a single medical consultation. It strictly demands a coordinated, multidisciplinary approach.
As advanced malignancies impact multiple physiological systems and profoundly affect the patient’s psychological stability, the supportive care team must consist of diverse clinical specialists.
Each professional brings a highly specific medical skill set to address the complex layers of physical and emotional suffering.
The Multidisciplinary Supportive Oncology Team
- Primary Oncologist: Directs the overall curative treatment strategy and ensures all palliative interventions safely align with the ongoing chemotherapy or surgical protocols.
- Palliative Care Physician: A board certified medical doctor who designs the comprehensive symptom management plan, focusing primarily on complex pharmacological pain control and complex medical decision making.
- Clinical Psychologist: Provides targeted cognitive behavioral therapy to manage severe clinical depression, anxiety disorders, and the profound emotional distress associated with the diagnosis.
- Clinical Dietitian: Formulates precise enteral or parenteral nutritional plans to aggressively combat cancer cachexia and manage severe treatment induced nausea.
Within this highly specialized collaborative unit, the role of palliative care nurse is absolutely central to the daily execution of the medical treatment plan.
This specialized nursing professional operates as the primary clinical touchpoint for the patient, spending the most direct, continuous time monitoring their physiological and emotional status in both inpatient and outpatient settings.
Core Clinical Responsibilities of the Palliative Care Nurse
- Continuous Symptom Assessment: The nurse conducts rigorous, daily clinical evaluations to quantify breakthrough pain levels, monitor respiratory function, and assess gastrointestinal stability. They immediately report any acute physiological exacerbations to the attending palliative physician for rapid pharmacological adjustment.
- Pharmacological Administration: They are strictly responsible for calculating, administering, and titrating complex intravenous analgesic medications and potent antiemetic drugs according to the precise orders of the medical team.
- Patient and Family Education: The nurse provides critical clinical education to the patient and their primary caregivers. They instruct families on proper surgical wound care, recognizing early physiological signs of systemic infection, and managing complex oral medication schedules safely in a home environment.
- Advance Care Planning Facilitation: They actively guide patients and families through the complex medical documentation required for advance directives, ensuring the patient’s exact long term care preferences are formally recorded and strictly honored by the entire hospital staff.
Maintaining continuous, direct clinical oversight, the specialized palliative care nurse ensures that the multidisciplinary care plan is flawlessly executed and rapidly adjusted to meet the patient’s dynamic daily requirements.
Finding Comprehensive Care: Palliative Care Units Near Me, Why Choose Dasappa Cancer Hospital
When patients and their families begin searching for local support systems, identifying a medical facility capable of managing both aggressive curative treatments and complex symptom control is absolutely paramount.
For those specifically seeking advanced palliative care units near me, Dasappa Cancer Hospital provides a premier, fully integrated clinical infrastructure.
Under the direct medical leadership of Dr. Pandu Dasappa, a highly distinguished surgical oncologist with over twenty seven years of clinical experience, our 75 bed super specialty facility consolidates all necessary supportive oncology services entirely under one roof.
We recognize that the financial implications of long term oncology treatment frequently cause significant distress for patients and their families.
Openly addressing the palliative care Bangalore cost requires absolute clinical and financial transparency. Dasappa Cancer Hospital strictly operates on an ethical, patient first philosophy.
We are dedicated to ensuring that advanced symptom management, expert nutritional planning, and comprehensive psychological support remain financially accessible without ever compromising the quality of medical care.
Choosing our facility for supportive oncology provides patients with several distinct clinical advantages:
- Dedicated Recovery Infrastructure: Immediate inpatient access to specialized intensive care units designed specifically to manage acute physiological exacerbations, severe respiratory distress, and intractable pain syndromes.
- Integrated Multidisciplinary Teams: Continuous on site access to board certified palliative physicians, specialized oncology nurses, clinical dietitians, and dedicated psychological counselors.
- Seamless Care Coordination: A highly unified clinical approach guaranteeing that all supportive pharmacological interventions strictly align with the patient’s primary surgical, chemotherapeutic, or radiation treatment plans.
Providing this level of comprehensive, multidisciplinary support, our medical team ensures that every patient maintains their highest possible quality of life throughout their oncology journey.
Conclusion
Integrating supportive oncology into a cancer treatment plan does not represent a cessation of active medical care.
Instead, it is a highly proactive, concurrent medical strategy designed to maintain the patient’s physiological strength and emotional resilience. By aggressively managing severe pain, preventing critical nutritional deficits, and addressing profound psychological distress, palliative care ensures that patients can safely and comfortably tolerate their life saving curative therapies.
If you or a family member require advanced symptom management alongside a primary oncology treatment plan, contact Dasappa Cancer Hospital today to schedule a comprehensive supportive care consultation and secure the multidisciplinary support you deserve.