Completing an intensive course of Chemotherapy treatment in Bangalore followed by a cellular infusion marks a major clinical milestone. Patients seeking care at a dedicated Cancer Hospital in Bangalore understand that the procedure itself is only the first phase of recovery.
As the Best Cancer Hospital in Bangalore, Dasappa Cancer Hospital prioritizes comprehensive post procedural care. A Stem cell transplant is a profound medical intervention that completely resets the patient’s biological and immunological baselines.
The period immediately following the infusion requires strict medical supervision and significant lifestyle modifications. Rebuilding a fully functional immune system from new hematopoietic cells is a gradual physiological process that extends far beyond the initial hospital discharge.
Patients must navigate profound immunosuppression, carefully monitor for systemic complications, and adhere to rigid environmental precautions to ensure successful cellular engraftment.
To prepare patients and their caregivers for this extended recovery phase, this clinical guide will detail the exact physiological expectations during survivorship, specifically focusing on the following critical areas:
- Immediate Physiological Milestones: We will outline the timeline for cellular engraftment and the strict isolation protocols required during the initial phase of profound neutropenia.
- Immunological Complication Management: We will explain the clinical protocols for monitoring and treating acute and chronic Graft Versus Host Disease following an allogeneic procedure.
- Long Term Lifestyle Modifications: We will detail the necessary dietary restrictions, physical rehabilitation strategies, and ongoing surveillance testing required to maintain long term disease remission.
Understanding the precise clinical realities of the recovery timeline, patients can actively participate in their post transplant care and safely navigate the transition from intensive treatment to permanent survivorship.
The Critical First 100 Days, Engraftment and Isolation
The immediate post transplant period, universally recognized in clinical oncology as the first 100 days, is the most highly monitored phase of the entire recovery timeline. Following the intravenous infusion of new hematopoietic stem cells, patients enter a temporary but highly dangerous physiological state known as profound neutropenia.
During this critical window, the high dose conditioning chemotherapy has completely eradicated the native immune system, but the newly infused stem cells have not yet established a functional biological presence within the bone marrow cavities.
According to clinical guidelines established by the National Cancer Institute, patients in this specific physiological state are exceptionally vulnerable to opportunistic bacterial, viral, and fungal infections.
Navigating this vulnerable period requires strict medical oversight, intense environmental isolation, and aggressive prophylactic interventions until the new immune system begins to function independently.
The primary clinical objective during this inpatient phase is achieving successful cellular engraftment. This vital biological milestone occurs when the infused stem cells successfully migrate into the skeletal marrow and begin synthesizing new, healthy blood components.
The multidisciplinary oncology team carefully manages this process through several rigorous protocols:
Continuous Hematological Monitoring
The medical team conducts daily complete blood counts to strictly track the patient’s absolute neutrophil count.
A sustained, consistent upward trajectory in new white blood cells provides the definitive clinical proof that the infused stem cells are actively proliferating and engrafting.
Prophylactic Pharmacotherapy
As the patient currently lacks the biological capacity to defend against common pathogens naturally.
Physicians administer a comprehensive, preemptive regimen of intravenous antiviral, antibacterial, and antifungal medications to prevent severe systemic infections.
Strict Environmental Isolation
Patients remain confined to specialized positive pressure hospital rooms equipped with High Efficiency Particulate Air filtration systems.
Stringent visitor restrictions, mandatory clinical masking, and rigorous hand hygiene protocols are universally enforced to eliminate any potential exposure to external environmental pathogens.
Routine Transfusion Support
The newly engraving stem cells prioritize the production of white blood cells for immune defense.
Until the marrow can independently produce adequate volumes of erythrocytes and thrombocytes, patients require frequent red blood cell and platelet transfusions to manage severe fatigue and prevent spontaneous internal hemorrhage.
Once the absolute neutrophil count reaches and maintains a safe clinical threshold for three consecutive days, the attending hematologist will officially confirm successful engraftment.
While this achievement typically allows the patient to be discharged from the strict isolation ward, the newly formed immune system remains highly immature, necessitating continued vigilance and strict lifestyle modifications as the recovery transitions to an outpatient setting.
Transplant with Donor Stem Cells
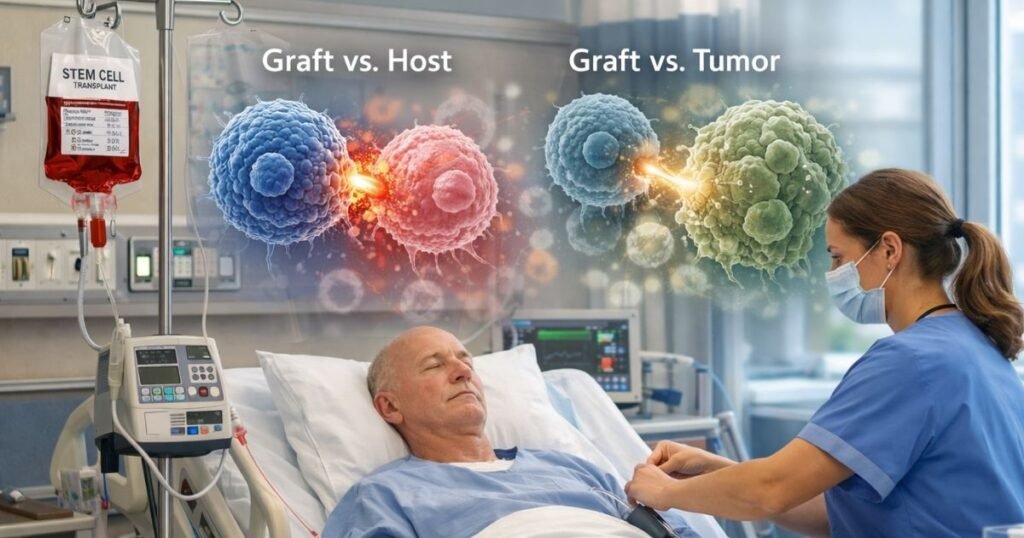
For patients undergoing a Transplant with donor stem cells, the recovery phase introduces an entirely unique set of biological variables.
Unlike an autologous procedure where the patient receives their own previously harvested cells, an allogeneic transplant establishes a completely foreign immune system within the patient’s body.
This new network of donor derived white blood cells must biologically integrate with the patient’s native organs and tissues.
According to comprehensive survivorship guidelines from the National Marrow Donor Program detailed in their Life After Transplant resources, managing this complex immunological integration is the primary focus of long term outpatient care.
The clinical hematology team must continuously monitor, evaluate, and medically balance two directly opposing biological phenomena:
The Graft Versus Tumor Effect (GVT)
This is the highly desired, curative benefit of an allogeneic procedure. The newly engrafted donor immune cells successfully identify the patient’s remaining microscopic cancer cells as foreign and aggressively destroy them.
This active immunological surveillance drastically reduces the statistical probability of a future disease relapse.
Graft Versus Host Disease (GVHD)
This represents the most significant systemic complication during the survivorship phase. In this scenario, the donor derived immune cells fail to recognize the patient’s healthy native tissues as safe.
Consequently, the new immune system mounts an inflammatory attack directly against the patient’s own organs.
To prevent severe organ damage, physicians prescribe a strict regimen of systemic immunosuppressive medications, such as cyclosporine or tacrolimus.
These potent drugs deliberately dampen the aggressiveness of the new immune system, allowing the donor cells to slowly build a tolerance to the host tissues.
Clinical oncologists classify Graft Versus Host Disease into two distinct categories based on the timeline of presentation and the specific organ systems targeted by the donor cells.
Clinical Classifications of Graft Versus Host Disease
| Pathological Classification | Standard Onset Timeline | Primary Organs Affected | Common Clinical Manifestations |
| Acute GVHD | Typically develops within the first 100 days following the cellular infusion. | Skin, Liver, and the Gastrointestinal Tract. | Severe maculopapular skin rashes, elevated hepatic bilirubin levels causing jaundice, severe watery diarrhea, and severe abdominal cramping. |
| Chronic GVHD | Typically develops after the first 100 days and can persist for several years. | Skin, Eyes, Mouth, Lungs, Joints, and Connective Tissues. | Extreme ocular dryness, mucosal ulcerations in the oral cavity, progressive joint stiffness, changes in skin pigmentation, and chronic respiratory inflammation. |
As the severity of these immunological reactions can fluctuate rapidly, patients must strictly adhere to their prescribed immunosuppressive pharmacological schedules.
Any sudden onset of cutaneous rashes, gastrointestinal distress, or respiratory difficulty strictly mandates an immediate clinical evaluation by the transplant team to adjust medication dosages and prevent irreversible tissue damage.
Long Term Physiological and Lifestyle Adjustments
Transitioning from the acute inpatient isolation ward to a standard home environment requires meticulous planning and strict adherence to new behavioral protocols.
As the newly engrafted immune system remains highly immature for twelve to twenty four months following the initial cellular infusion, patients must actively modify their daily routines.
These strict adjustments are clinically necessary to mitigate the ongoing risk of severe systemic infections and properly manage the chronic physiological side effects of the high dose conditioning chemotherapy.
The long term recovery phase demands a highly structured approach to daily living. The multidisciplinary oncology team provides patients with a comprehensive set of non negotiable lifestyle modifications tailored to their specific state of profound immunosuppression.
Mandatory Post Transplant Lifestyle Protocols
| Clinical Focus Area | Required Patient Modification | Primary Medical Rationale |
| Nutritional Intake | Strict adherence to a neutropenic diet, ensuring all food is thoroughly cooked to exact thermal temperatures while absolutely avoiding all raw produce, undercooked meats, and unpasteurized dairy products. | To completely eliminate the introduction of foodborne bacterial and fungal pathogens into the highly vulnerable and frequently ulcerated gastrointestinal tract. |
| Physical Rehabilitation | Implementing a customized, highly gradual physical therapy regimen under the direct supervision of an oncology rehabilitation specialist. | To safely counteract the severe muscular atrophy and profound chronic fatigue induced by prolonged bed rest and myeloablative conditioning without triggering dangerous cardiopulmonary stress. |
| Environmental Hygiene | Enforcing rigorous hand washing protocols, completely avoiding large public crowds, and strictly isolating from any individuals exhibiting symptoms of contagious respiratory illnesses. | To minimize direct exposure to common environmental pathogens and viral vectors during the prolonged phase of immune system maturation. |
| Immunological Reconstitution | Following a strict clinical schedule to receive entirely new doses of standard childhood and adult vaccinations, typically beginning one year post transplant. | To reestablish active systemic immunity to preventable diseases, as the high dose chemotherapy permanently erased the patient’s previous vaccine acquired immunological memory. |
In addition to these physical protocols, patients must also manage the chronic dermatological and mucosal side effects resulting from the systemic toxicity of the cancer treatments.
Utilizing specialized, hypoallergenic skincare products and maintaining rigorous oral hygiene are essential daily practices to prevent localized bacterial infections in compromised barrier tissues. Strictly committing to these extensive lifestyle adjustments, patients actively protect their newly developing immune systems and significantly accelerate their overall physiological recovery.
Monitoring Disease Remission
The transition into long term survivorship does not signify the end of medical care. Following a successful stem cell transplant for cancer, patients enter a mandatory phase of rigorous, scheduled clinical surveillance.
The primary objective of this ongoing monitoring is to confirm continuous disease remission, detect any early signs of a cancer relapse, and aggressively manage the late physiological effects of the high dose conditioning regimens.
The frequency of oncology consultations is highest during the first year and gradually decreases as the patient demonstrates sustained biological stability.
During these critical follow up visits, the multidisciplinary medical team relies on highly specific diagnostic protocols to comprehensively evaluate the patient’s ongoing hematological health.
Standard Diagnostic Surveillance Protocols
| Diagnostic Modality | Primary Clinical Purpose | Standard Monitoring Timeline |
| Complete Blood Count (CBC) | To quantify the exact levels of circulating red blood cells, white blood cells, and platelets, guaranteeing the newly engrafted marrow maintains healthy systemic production. | Highly frequent during the first year, gradually tapering to routine annual evaluations. |
| Bone Marrow Biopsy | To physically extract and microscopically examine the cellular architecture within the marrow cavity, strictly ruling out the return of malignant cells. | Conducted at precise clinical milestones, typically at day 100, six months, and one year post procedure. |
| Chimerism Analysis | Utilized strictly following a Transplant with donor stem cells to calculate the exact percentage of donor immune cells versus native host cells currently circulating in the bloodstream. | Performed routinely during the first year to confirm full donor engraftment and predict the risk of early relapse. |
| Comprehensive Metabolic Panel | To evaluate the ongoing filtration capacity of the kidneys and the enzymatic function of the liver, monitoring for delayed organ toxicity. | Conducted concurrently with routine blood counts during scheduled oncology visits. |
Beyond strictly monitoring the original malignancy, the long term survivorship protocol mandates routine screening for secondary cancers.
The intense total body radiation and high dose chemotherapy utilized during the initial myeloablative conditioning phase statistically increase the patient’s lifetime risk of developing new, unrelated malignancies.
Furthermore, patients require specialized annual cardiopulmonary evaluations, including echocardiograms and pulmonary function tests, to detect any delayed structural toxicity to the heart muscle or respiratory tissues.
Maintaining absolute compliance with this extensive, lifelong surveillance schedule, patients ensure that any delayed physiological complications or microscopic signs of disease relapse are identified and aggressively treated at the earliest possible stage.
Why Choose Dasappa Cancer Hospital? Comprehensive Survivorship Care at Dasappa Cancer Hospital
Successfully navigating the long term recovery phase of a hematopoietic cellular infusion requires far more than standard outpatient monitoring.
It demands a highly coordinated, multidisciplinary approach to manage complex immunological shifts and prevent systemic complications. Dasappa Cancer Hospital provides an elite clinical infrastructure specifically designed to support patients through every stage of this rigorous survivorship journey.
Under the expert leadership of Dr. Pandu Dasappa, a premier oncologist with over twenty seven years of clinical experience, our 75 bed super specialty facility consolidates all necessary post transplant care strictly under one roof.
Our dedicated survivorship program features several critical clinical advantages:
- Dedicated Intensive Care: Our specialized ICU and recovery wards are fully equipped to rapidly manage acute immunological complications or severe opportunistic infections should they arise during the outpatient phase.
- Advanced Diagnostic Imaging: We maintain state of the art laboratory and radiology departments to facilitate the strict, high frequency surveillance testing required to confirm ongoing disease remission.
- Integrated Supportive Therapies: We provide continuous access to clinical nutritionists, targeted pain management specialists, and dedicated physical rehabilitation teams to actively rebuild physiological strength and manage chronic fatigue.
- Psychosocial Oncology Support: Recognizing the profound emotional toll of an extended recovery, our facility offers comprehensive psychological counseling to support the mental well being of both patients and their primary caregivers.
Combining advanced medical technology with a deeply compassionate, patient first philosophy, our oncology team ensures that every patient receives the precise clinical oversight required to achieve a permanent hematological recovery.
Conclusion
A stem cell transplant represents a highly intensive but profoundly curative medical intervention for severe hematological malignancies.
While the recovery timeline is gradual and strictly demands significant lifestyle modifications, achieving full cellular engraftment provides a definitive pathway to long term survivorship. By closely partnering with a dedicated multidisciplinary oncology team and maintaining absolute compliance with environmental and surveillance protocols, patients can successfully rebuild their immune systems and reclaim their physiological health.
If you are preparing for an advanced hematological procedure or require expert post transplant care, contact Dasappa Cancer Hospital today to schedule a comprehensive clinical consultation and secure your path to recovery.